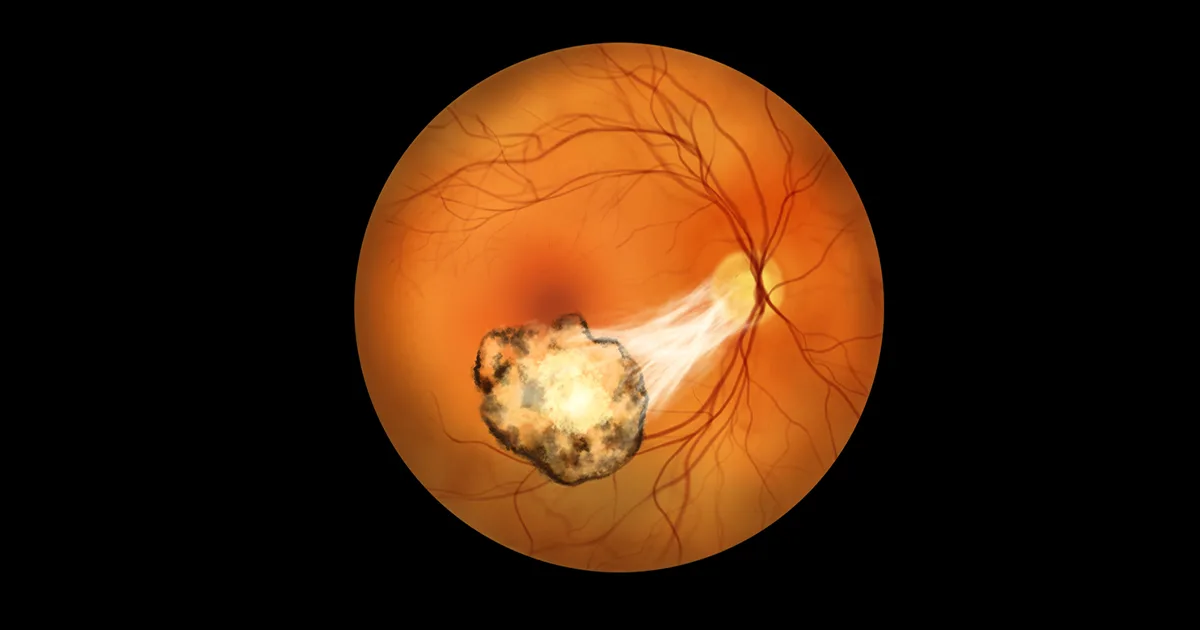
The choroid is a spongy vascular layer between the retina and the white of the eye. It nourishes the outer retina and regulates temperature. When it becomes inflamed, the condition is called choroiditis. Often part of a broader inflammatory process inside the eye called uveitis, choroiditis can threaten vision if not promptly diagnosed and treated.
This guide walks you through what choroiditis is, its common causes, symptoms, and treatment options.
What Is Choroiditis?
Choroiditis is inflammation of the choroid. Because the choroid supports the outer retina, inflammation here often involves the retina too, producing chorioretinitis. Choroiditis is commonly classified under posterior or panuveitis depending on extent.
Posterior uveitis
Inflammation mainly in the choroid and retina.
Panuveitis
Inflammation throughout the eye (anterior, intermediate, and posterior).
What Causes Choroiditis?
Infectious causes
- Tuberculosis (common in India)
- Toxoplasmosis
- Syphilis
- Viral infections (herpes, CMV)
- Fungal infections
- Bartonella (cat-scratch disease)
- Histoplasmosis in certain regions
Autoimmune and inflammatory causes
- Sarcoidosis
- Vogt-Koyanagi-Harada (VKH) disease
- Behçet disease
- Sympathetic ophthalmia
- Multiple sclerosis-associated uveitis
Isolated eye disorders
- Serpiginous choroiditis
- Multifocal choroiditis and panuveitis (MCP)
- Acute posterior multifocal placoid pigment epitheliopathy (APMPPE)
- Birdshot chorioretinopathy
Masquerade syndromes
- Intraocular lymphoma
- Leukaemia
- Metastatic cancer
Idiopathic
Sometimes the cause cannot be identified despite tests.
What Are the Symptoms of Choroiditis?
- Blurred vision
- Dark or floating spots in the visual field
- Flashes of light
- Central or paracentral blind spots
- Reduced contrast sensitivity
- Mild to moderate pain
- Redness in some cases
- Light sensitivity
- Sometimes reduced colour vision
Symptoms depend on the extent, location, and type of choroiditis.
How Is Choroiditis Diagnosed?
A structured work-up at an eye specialist hospital includes:
- Detailed history (infections, travel, systemic conditions)
- Visual acuity and refraction
- Slit-lamp examination
- Dilated fundus examination
- OCT of the retina and choroid (enhanced-depth imaging)
- Fluorescein and indocyanine green angiography
- Blood tests (Mantoux, QuantiFERON, syphilis, ACE, ANA, HLA typing)
- Imaging (chest X-ray, HRCT chest, MRI brain)
- Sometimes vitreous sampling or biopsy in suspicious cases
Identifying the cause guides treatment.
How Is Choroiditis Treated?
Treatment depends on the cause and severity.
1. Corticosteroids
The backbone of anti-inflammatory treatment.
- Topical drops
- Peribulbar or intravitreal injections
- Oral steroids
- Intravenous steroids for severe cases
2. Immunosuppressive therapy
- Methotrexate
- Azathioprine
- Mycophenolate
- Cyclosporine
- Used in chronic, recurrent, or steroid-dependent cases
3. Biologic therapy
- Anti-TNF agents (infliximab, adalimumab)
- For selected autoimmune uveitis cases
4. Antimicrobial therapy
- Antitubercular therapy for ocular TB
- Antivirals for herpes viruses
- Anti-parasitic drugs for toxoplasmosis
- Antibiotics for bacterial causes
- Antifungals for fungal cases
5. Treatment of underlying systemic disease
Coordinated care with rheumatology, infectious disease, or internal medicine specialists.
6. Supportive measures
Sunglasses for photosensitivity, lubricating drops, and prescribed eye treatments as needed.
7. Surgery
Rare. May be needed for complications such as macular oedema, cataract, vitreous haemorrhage, or retinal detachment.
Complications of Choroiditis
- Cystoid macular oedema
- Cataract
- Glaucoma (steroid-induced or inflammatory)
- Retinal detachment
- Choroidal neovascularisation
- Optic nerve damage
- Permanent vision loss
Regular follow-up with retinal imaging helps catch these early.
Is Choroiditis Serious?
Yes, it can be serious. Untreated or poorly controlled choroiditis can cause permanent vision loss. However, with early diagnosis, targeted therapy, and regular follow-up, many patients maintain useful vision. The seriousness depends on the cause, extent, and response to treatment.
How Serious Is Eye Inflammation?
Eye inflammation ranges from mild anterior uveitis, often easily controlled with drops, to severe panuveitis or infective posterior uveitis that can threaten vision. Key principles:
- Any new, painful, red, or vision-affecting eye deserves prompt review
- Chronic or recurrent inflammation needs structured specialist care
- Systemic conditions often drive eye inflammation
- Long-term management is essential for chronic cases
- Steroid use requires careful monitoring
How to Manage Eye Inflammation Safely
- Never self-start steroid drops
- Follow prescribed drop schedules strictly
- Attend all follow-up visits
- Inform the doctor of any systemic symptoms
- Take systemic medicines on time
- Report new floaters, flashes, or vision drop immediately
- Keep up supportive care: lubricants, sunglasses, lid hygiene
- Coordinate with physicians for TB, autoimmune, or infectious conditions
Choroiditis in Special Groups
Children
Usually needs paediatric rheumatology and ophthalmology coordination. Juvenile idiopathic arthritis and some infections are common causes.
Pregnant women
Medication choices are tailored carefully; steroids with caution.
Immunocompromised patients
CMV, toxoplasma, and opportunistic infections are more likely.
Older adults
Autoimmune conditions, masquerade syndromes, and vascular contribution to choroidal health become important.
Follow-up
- Frequent during acute treatment
- Monthly for stable cases on immunosuppressive therapy
- Every 3-6 months for well-controlled chronic cases
- Vision checks, eye pressure, fundus imaging, and systemic review on each visit
Prevention and Lifestyle Tips
- Treat systemic infections promptly
- Manage autoimmune conditions with your rheumatologist
- Vaccinate against vaccine-preventable infections
- Get regular eye checks if you have chronic systemic disease
- Avoid risky behaviours that increase infection risk
- Practice good hygiene and pet safety for toxoplasmosis prevention
- Manage TB contact risk
- Stop smoking
When Should You See a Doctor?
Urgent review if:
- Sudden blurring or vision loss
- Severe eye pain
- Significant light sensitivity
- Flashes and many floaters
- Headache with eye symptoms
- Systemic symptoms with eye involvement
- Recurrent uveitis that worsens
Routine review for:
- Ongoing uveitis on medication
- Side-effect monitoring of steroids and immunosuppressives
- Follow-up retinal imaging
- Control of underlying systemic disease
Choroiditis Care at Vasan Eye Care
Vasan Eye Care has been looking after patients across India since 2002, now as part of ASG Enterprises. With more than 150 super-speciality centres, 500+ ophthalmologists, and over 5,000 trained eye care staff, the team handles inflammatory eye conditions through detailed imaging, systemic work-up, and structured retinal disease treatment and uveitis care pathways. An eye hospital in the network coordinates with physicians for underlying systemic conditions.
Key Takeaways
Early diagnosis and regular follow-up protect vision.
Choroiditis is inflammation of the choroid, often with retinal involvement.
Causes include infections (TB, toxoplasma, syphilis, viruses), autoimmune disease, and isolated conditions.
Symptoms include blurred vision, floaters, flashes, and blind spots.
Diagnosis involves eye imaging, blood tests, and systemic investigations.
Treatment combines steroids, immunosuppressives, and cause-specific therapy.
Frequently Asked Questions (FAQs)
Treatment depends on the underlying cause. Infectious choroiditis needs specific antimicrobial therapy. Autoimmune cases respond to steroids and immunosuppressives or biologic agents. Supportive care includes lubricating drops, sunglasses, and treatment of complications like macular oedema and cataract. Regular follow-up and coordinated care with rheumatologists and physicians support long-term control.
Yes, it can be. Untreated choroiditis can cause permanent vision loss through complications like macular oedema, choroidal neovascularisation, glaucoma, and retinal damage. Early diagnosis and appropriate treatment usually preserve vision. The seriousness depends on the cause, extent, and response to therapy. Regular specialist follow-up is essential.
The right treatment depends on the cause and severity. Anterior uveitis often responds to steroid eye drops and cycloplegics. Intermediate, posterior, and panuveitis may need oral steroids, injections, or immunosuppressive therapy. Infectious causes need targeted antimicrobials. A specialist examines, investigates, and prescribes tailored therapy rather than relying on any single broad approach.
Eye inflammation ranges from mild and self-limiting to severe and vision-threatening. Painful red eyes with blurred vision, uveitis with floaters and flashes, and systemic symptoms combined with eye changes all need prompt specialist review. Chronic and recurrent inflammation requires long-term management and specialist follow-up to preserve vision.
References
- American Academy of Ophthalmology. Uveitis. https://www.aao.org/eye-health/diseases/what-is-uveitis
- National Center for Biotechnology Information. Choroiditis. https://www.ncbi.nlm.nih.gov/books/NBK580534/
- National Eye Institute. Uveitis. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/uveitis
- WebMD. Uveitis. https://www.webmd.com/eye-health/uveitis