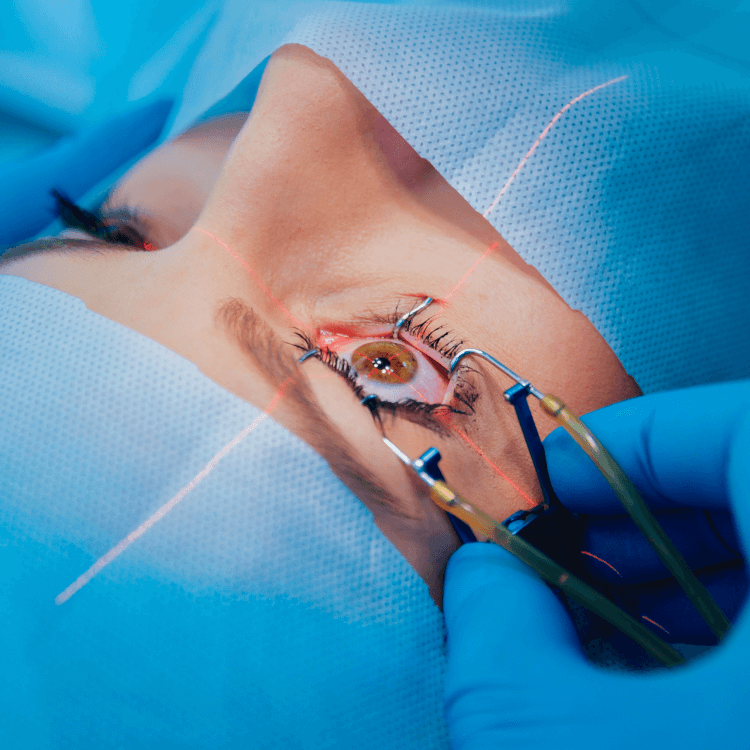
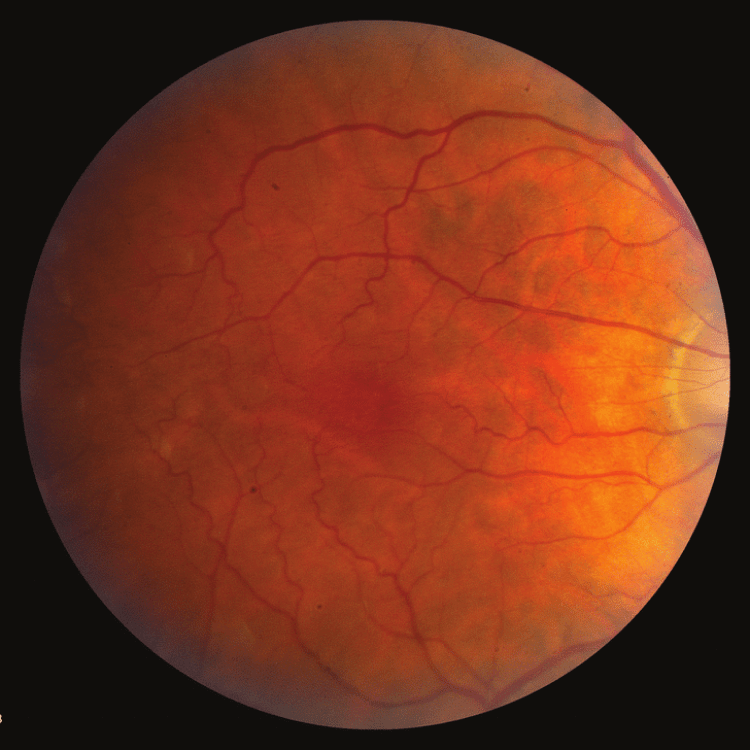
Retinal Detachment
What is Retinal Detachment?
The retina is a thin layer at the back of the eye that captures light and sends signals to the brain, helping us see. Retinal detachment occurs when this layer separates from the eye wall, cutting off its blood supply and stopping it from functioning. It causes sudden vision loss and is painless, making it a serious condition that requires urgent attention.
Understanding Retinal Detachment
Picture wallpaper peeling away from a wall. The wallpaper is still there, it has just separated from the surface it was attached to. That is essentially what happens in a retinal detachment. The retina, which should be lying flat and firmly against the back of the eye, lifts away either because of a tear that lets fluid in underneath it, because scar tissue pulls it, or because fluid pushes it up from below.
Once the retina detaches, the cells in it begin to deteriorate without their blood supply. The longer the detachment goes untreated, the more permanent the damage becomes. If the central part of the retina, called the macula, gets involved, central vision can be affected even after successful treatment.
Retinal detachment is not something that happens gradually and gives you months to decide. It often unfolds over hours to days. This is why recognising the early signs quickly and acting on them makes such a significant difference to how much vision can be saved.
What are the Symptoms of Retinal Detachment?
The retinal detachment symptoms are usually very sudden and quite distinctive once you know what to look for. The retinal detachment symptoms do not include pain, which is what catches many people off guard. Because the eye does not hurt, some people put off seeing a doctor for a few days, not realising how quickly the situation can worsen.
Symptoms of Retinal Detachment to Watch For
| Symptom | What it feels like |
| Sudden flashes of light | Brief flickers or streaks of light at the edges of vision, especially in dim settings |
| A sudden increase in floaters | New dark spots, threads, cobwebs, or squiggly lines drifting across the vision |
| A shadow or curtain | A dark area spreading from one side of the vision, like a curtain being drawn across |
| Blurred vision | Objects appear less sharp, particularly in one specific part of the visual field |
| Vision getting worse quickly | A noticeable and rapid deterioration in what one eye can see |
Are a Few Floaters Normal?
Yes, occasional floaters are normal and very common, especially in people over 40 or those with high spectacle numbers. The key is the sudden change. If you have always had a couple of floaters and nothing has changed, that is usually not a cause for concern. But if you suddenly notice a shower of new floaters, or floaters you have never seen before, particularly alongside flashes of light, that combination is a warning sign that needs same-day attention.
When Should You Go to an Eye Doctor?
Please visit an eye specialist urgently if you notice:
• A sudden increase in floaters or new floaters appearing out of nowhere
• Flashes of light that keep coming back, especially in dim light or when moving your eyes
• A shadow or dark area covering any part of your vision
• Any rapid, unexplained change in vision in one eye
• The above symptoms appearing after an eye injury or recent eye surgery
There is no version of these symptoms where waiting to see if they improve on their own is a safe choice.
What are the Types of Retinal Detachment?
Understanding the types of retinal detachment helps explain why the condition can happen in people of different ages and health backgrounds. The different types of retinal detachment differ in how and why the retina separates, which also influences the approach to retinal detachment treatment.
The Three Types of Retinal Detachment
1. Rhegmatogenous (Tear-related) This is the most common type of retinal detachment, and the one most people are referring to when they say “detached retina.” As we get older, the gel-like fluid inside the eye (called the vitreous) slowly shrinks and may tug on the retina as the eye moves. If this tugging creates a tear, fluid can seep through the tear and get underneath the retina, gradually pushing it away from the eye wall. People with high myopia (shortsightedness) are at greater risk because their eyes are longer and the retina is stretched more thinly.
2. Tractional (Scar tissue pulling) In this type, scar tissue that has formed on the surface of the retina pulls it away from the back of the eye. Diabetic eye disease (diabetic retinopathy) is the most common cause of this type in India. When blood sugar is poorly controlled over many years, it damages the tiny blood vessels in the retina and can cause abnormal new blood vessels and scar tissue to grow. As the scar tissue tightens over time, it pulls the retina with it.
3. Exudative (Fluid buildup without a tear) In this rarer type, fluid accumulates underneath the retina without any tear or break in the retina itself. The fluid pushes the retina forward and away from the eye wall. This can happen because of inflammation inside the eye, certain tumours, or leaking blood vessels. Because there is no tear, the treatment approach is different from the other two types.
Types of Retinal Detachment at a Glance
| Type | What causes it | Who is most at risk |
| Rhegmatogenous | A tear in the retina that lets fluid in | People over 40, high myopia, previous eye surgery |
| Tractional | Scar tissue pulling the retina away | Diabetic patients, those with proliferative retinopathy |
| Exudative | Fluid buildup under the retina, no tear | Inflammatory eye conditions, certain tumours |
What are the Causes of Retinal Detachment?
The causes of retinal detachment vary depending on the type involved. In some cases, age is the main factor. In others, it is an underlying health condition like diabetes or high myopia. Understanding the causes of retinal detachment helps identify who needs to be more watchful, and who should be having regular eye check-ups even when their vision seems fine.
Common Causes and Risk Factors
Age-related vitreous changes: As people get older, the vitreous gel inside the eye naturally shrinks and becomes more watery. As it does this, it can pull away from the retina. In most cases this happens without any problem. But in some people, the vitreous pulls strongly enough to create a tear, and that tear can lead to a retinal detachment. This is one of the most common causes of retinal detachment in people over the age of 50.
High myopia (shortsightedness): People with a high spectacle number for myopia have longer eyeballs than average. This extra length means the retina is stretched more thinly across the back of the eye, making it more prone to tearing. In India, where myopia rates are rising significantly among school-age children, this is an increasingly relevant risk factor for retinal detachment in younger adults.
Diabetes: Poorly controlled diabetes damages the blood vessels in the retina over time. In advanced diabetic eye disease, abnormal new blood vessels grow along with scar tissue. This scar tissue can contract and pull the retina away from the back of the eye, causing a tractional retinal detachment. This is one of the most common causes of retinal detachment in India due to the country’s high diabetes burden.
Previous eye surgery or injury: Anyone who has had cataract surgery, glaucoma surgery, or any other eye operation has a slightly elevated risk of retinal detachment, particularly in the months following the procedure. A significant blow or injury to the eye can also cause a retinal tear or detachment directly.
Family history: If a parent or sibling has had a retinal detachment, the risk is somewhat higher. If the other eye of a person who has already had a retinal detachment has not been checked, it should be, because that eye carries an increased risk too.
Previous retinal tears or thinning: Some people have areas of thinning in their retina, called lattice degeneration, which can sometimes be spotted during a routine eye examination before any detachment has occurred. These areas are more prone to tearing and can sometimes be treated preventively.
Causes of Retinal Detachment: Summary
| Cause | Who it affects most |
| Age-related vitreous changes | People over 50 |
| High myopia | Younger adults, especially those with power above -6 |
| Diabetic eye disease | People with long-standing or poorly controlled diabetes |
| Eye surgery or injury | Anyone post-surgery or with a history of eye trauma |
| Family history | Those with a first-degree relative with retinal detachment |
| Lattice degeneration | Often found incidentally during eye check-ups |
How Do Doctors Diagnose Retinal Detachment?
Diagnosing a retinal detachment is done through a detailed eye examination. The doctor needs to look at the back of the eye directly to see the retina, assess the extent of any detachment, and identify the location and number of any tears.
How the Eye is Examined
| Step | What it involves |
| Dilated eye examination | Eye drops widen the pupil so the doctor can get a clear view of the retina through an ophthalmoscope |
| Slit lamp examination | A detailed look at the front and middle parts of the eye, and the periphery of the retina with a specialised lens |
| Indirect ophthalmoscopy | A bright light and a hand-held lens used to examine the full retina, including the far edges where tears most commonly occur |
| Ultrasound scan of the eye | Used when the view of the retina is blocked, for example by a dense cataract or bleeding inside the eye |
| OCT (Optical Coherence Tomography) | A scan that gives a detailed cross-section image of the retina layers, helpful in assessing the macula |
The examination requires the pupils to be dilated with eye drops, so vision will be blurry for a few hours afterwards. Patients should bring someone to drive them home if possible.
What Does Retinal Detachment Treatment Look Like?
Retinal detachment treatment depends on the type of detachment, how far it has spread, whether the central part of the retina (the macula) is involved, and how long it has been present. The goal of all forms of retinal detachment treatment is to reattach the retina securely and restore as much vision as possible.
It is important to understand that the sooner retinal detachment treatment is received, the greater the chance of a good visual outcome. If the macula has not yet detached at the time of treatment, there is a much higher chance of recovering good central vision. Once the macula detaches, central vision is harder to recover fully.
Retinal Detachment Treatment Options
1. Laser Treatment (Photocoagulation): For retinal tears before full detachment If a tear in the retina is caught before it has caused a full detachment, laser treatment can seal it and prevent fluid from getting underneath the retina. The laser creates small burns around the tear that form a scar, bonding the retina firmly to the underlying tissue. This retinal detachment treatment is done in a clinic, takes only a few minutes, and does not require hospitalisation. It is one of the reasons why regular eye check-ups matter so much for high-risk individuals.
2. Cryotherapy (Freeze Treatment): For tears, similar to laser Cryotherapy uses a cold probe applied to the outside of the eye to create the same type of bonding scar around a retinal tear. It is sometimes preferred over laser in certain locations on the retina where laser access is more difficult. Like laser, this is used for tears or very early detachments.
3. Pneumatic Retinopexy: For suitable, early detachments In this procedure, a small gas bubble is injected into the eye. The bubble floats up and pushes against the detached area of the retina from the inside, pressing it back against the eye wall. The patient needs to maintain a specific head position for several days to keep the bubble over the detachment. Laser or cryotherapy is then used to seal the tear. Not all detachments are suitable for this approach, and the patient’s ability to maintain the required head position is an important factor.
4. Scleral Buckle Surgery: Established surgical treatment A scleral buckle is a small piece of silicone material that is sutured to the outside of the eyeball. It gently indents (buckles) the eye wall inward, relieving the pulling force that caused the retina to detach, and bringing the eye wall closer to the detached retina. Laser or cryotherapy is also applied to seal the tear. This procedure is done under anaesthesia and requires a short recovery period. It has been used successfully for decades and remains an important option in retinal detachment treatment.
5. Vitrectomy: For complex or extensive detachments Vitrectomy is the most common surgical retinal detachment treatment for complex cases, including tractional detachments from diabetic eye disease, large or multiple tears, and detachments involving the macula. The surgeon removes the vitreous gel from inside the eye and may peel any scar tissue off the retina. The retina is then pushed back into position using a laser, and the eye is filled with either a gas bubble or silicone oil to hold the retina in place while it heals. Patients who receive a gas bubble need to maintain a specific head position for a period after surgery. Those who receive silicone oil may need a second operation to remove it at a later date.
Retinal Detachment Treatment at a Glance
| Treatment | When it is used | Setting |
| Laser photocoagulation | Retinal tear, before full detachment | Outpatient clinic |
| Cryotherapy | Retinal tear in certain locations | Outpatient clinic |
| Pneumatic retinopexy | Early, suitable detachments | Minor procedure |
| Scleral buckle | Moderate detachments, younger patients | Surgery under anaesthesia |
| Vitrectomy | Complex, large, or tractional detachments | Surgery under anaesthesia |
Related Eye Conditions
- Diabetic Retinopathy
- Posterior Vitreous Detachment
- Lattice Degeneration
- Macular Degeneration
- High Myopia (Pathological)
References
Cleveland Clinic. Retinal Detachment: Symptoms, Causes and Treatment. Last reviewed 2023. https://my.clevelandclinic.org/health/diseases/10705-retinal-detachment
Mayo Clinic. Retinal Detachment: Diagnosis and Treatment. Last reviewed 2023. https://www.mayoclinic.org/diseases-conditions/retinal-detachment/diagnosis-treatment/drc-20351348
American Academy of Ophthalmology. Detached Retina. Published December 2025. https://www.aao.org/eye-health/diseases/detached-torn-retina
Mitry D, Charteris DG, Fleck BW, et al. The epidemiology of rhegmatogenous retinal detachment: geographical variation and clinical associations. British Journal of Ophthalmology. 2010;94(6):678-684. https://pmc.ncbi.nlm.nih.gov/articles/PMC2405853/
NYU Langone Health. Procedures to Treat Retinal Tears and Retinal Detachments. https://nyulangone.org/conditions/retinal-detachment/treatments/procedures-to-treat-retinal-tears-retinal-detachments
For appointments, call 1800 571 2222 or visit your nearest Vasan Eye Care centre.
What Happens If Retinal Detachment Is Not Treated?
If a retinal detachment is left without treatment, the retina continues to separate further from the eye wall. The cells of the retina gradually die without their blood supply, and this damage cannot be reversed. Over days to weeks, the entire retina may detach, resulting in complete and permanent loss of vision in that eye.
Even a partial retinal detachment that initially affects only the side vision can progress to involve the macula, the central part of the retina responsible for detailed, sharp vision. Once the macula is involved, recovering good central vision becomes much harder, even with the most successful surgical repair.
The message is straightforward. If the symptoms appear, see an eye doctor the same day.
Retinal Detachment and Diabetes: Why Indian Patients Need to Know
India has one of the largest populations of people with diabetes in the world. Diabetic eye disease is one of the causes of retinal detachment that is most specific to this context, and it deserves special attention.
In diabetic retinopathy, the tiny blood vessels of the retina are damaged by years of high blood sugar. In advanced cases, abnormal new blood vessels grow along the retina and into the vitreous. These fragile vessels bleed easily, and the scar tissue they leave behind can pull the retina away from the back of the eye, causing a tractional retinal detachment.
The important thing to know is that diabetic eye disease can be monitored and managed. Regular retinal screening is recommended at least once a year for anyone with diabetes, even if their vision seems completely normal. Early stages of retinal disease often have no symptoms. By the time vision changes are noticed, significant damage may already have occurred. Laser treatment and injections can slow or prevent the progression to retinal detachment in many patients if started at the right time.
If you have diabetes and have not had a dilated retinal examination in the past year, this is a good time to book one.
Retinal Detachment and High Myopia in India
Myopia, or shortsightedness, is increasing at a striking rate in India and across Asia. Children are developing myopia younger, and the average spectacle number is getting higher. This matters for retinal health because high myopia stretches the retina over a longer eyeball, making it thinner and more prone to developing tears and holes.
A person with a spectacle number of -6 or higher has a significantly elevated risk of retinal tears and detachment compared to someone with normal vision or mild myopia. Regular dilated eye examinations are recommended for anyone with high myopia, even if they are young and have no symptoms.
If a retinal tear is found during an examination before it has caused a detachment, laser treatment can seal it quickly and prevent a detachment from developing. This is one of the clearest examples of how a routine eye check-up can protect long-term vision.
Retinal Care at Vasan Eye Care
Retinal detachment requires prompt, skilled care, and it is a condition our team at Vasan Eye Care sees and manages regularly. At Vasan Eye Care, retinal services are a core part of what we do across our network of 150+ centres in India. Our retinal specialists are trained in the full range of diagnostic and surgical options for managing retinal detachment.
When you come to us with retinal symptoms, here is what you can expect:
- A thorough dilated eye examination on the same visit, without being turned away or asked to come back later
- A clear explanation of what is happening with your retina and what the options are
- Access to laser treatment, vitrectomy, and other surgical procedures at our equipped centres
- Honest, straightforward guidance on the likely outcome based on your specific situation
- Follow-up care to monitor the retina after treatment and check the other eye
Our 500+ eye care specialists are part of ASG Enterprises, India’s largest eye care network. We are committed to making quality retinal care accessible across India, including in cities and towns that may not have had access to this level of care before.
Simple Guide to Retinal Detachment Terms
| Word or phrase | What it means in simple terms |
| Retina | The light-sensitive layer at the back of the eye that allows us to see |
| Vitreous | The gel-like fluid that fills the inside of the eye |
| Floaters | Dark spots, threads, or shapes that drift across the vision |
| Macula | The central part of the retina responsible for sharp, detailed vision |
| Rhegmatogenous detachment | The most common type, caused by a tear in the retina |
| Tractional detachment | Caused by scar tissue pulling the retina away, often from diabetes |
| Exudative detachment | Caused by fluid building up under the retina without a tear |
| Laser photocoagulation | A laser treatment that seals retinal tears |
| Vitrectomy | Surgery to remove the vitreous gel and repair the retina |
| Scleral buckle | A band placed on the outside of the eye to support the detached retina |
| Gas bubble | Injected into the eye to hold the retina in position during healing |
Symptoms
How to know if your Retina is detached


Sudden increase in floaters

Ring of floaters

Sensation of veil-like or curtain over vision
Distorted vision

Central visual loss
Risk Factors
Common risk factors of Retinal Detachment
Treatments Available
Here’s how our experts treat it
At Vasan, once the diagnosis is made, the doctor recommends retinal surgeries depending on the type and severity of the detachment. The treatments include:
Retinal Laser Photocoagulation
Laser surgery seals or reattaches the retina by scarring the area around the detachment or tear.
Cryopexy
Cryopexy repairs retinal tears by applying intense cold therapy to the back of the eye using a specialised probe, which creates scar tissue around the tear.
Pneumatic Retinopexy
This process involves using gas or air bubble injection into the vitreous cavity that pushes against the retinal hole, stopping fluid flow and allowing the retina to reattach.
Scleral Buckling
Scleral buckling involves securing a piece of silicone band or sponge to the sclera, the white part of your eye. This action helps reattach the retina by pushing it back into its supportive tissues.
Vitrectomy
Vitrectomy is an advanced surgery done by our specialists to remove the gel-like substance called ‘vitreous humour’ from inside your eye. This helps them get better access to your retina.
Frequently Asked Questions (FAQs)
There is no single answer because it depends on the type, location, and how far the detachment has spread. For tears caught early, laser or freeze treatment works very well. For a full detachment, surgery is needed, and vitrectomy is currently the most widely used surgical approach for complex cases, while scleral buckle remains an established option for certain types. The outcome of retinal detachment treatment is closely tied to how quickly care is sought after symptoms first appear.
For small tears or very early detachments that have not yet become full detachments, laser treatment or cryotherapy can seal the tear and prevent it from progressing, without any surgical incision. However, once a proper retinal detachment has occurred, surgery is almost always needed. There are no medicines or eye drops that can reattach a detached retina. The only exception is some cases of exudative detachment caused by inflammation, where treating the underlying inflammation may resolve the fluid build-up.
Yes, in most cases. Advances in retinal surgery over the past few decades mean that the large majority of retinal detachments can be successfully repaired. The key question is not just whether the retina can be reattached, but how much useful vision will be recovered. If treatment is received before the macula detaches, there is a very good chance of recovering good central vision. If the macula has been off for more than a day or two, central vision may not fully return even after a technically successful operation. This is why speed matters so much.
It is very serious. Without treatment, a retinal detachment will almost always result in permanent vision loss or complete blindness in the affected eye. Even with treatment, visual outcomes depend heavily on the timing and extent of the detachment. That said, with modern surgical options, the majority of patients who receive prompt retinal detachment treatment recover vision that allows them to function normally in daily life. The seriousness should not cause panic, but it should motivate immediate action.
Yes, it can, though most cases affect only one eye. However, if one eye has had a retinal detachment, the other eye has a higher risk too. This is why doctors always examine both eyes carefully after a detachment is found in one eye, even if the other eye seems fine. People who have had a detachment in one eye should also report any new visual symptoms in the other eye immediately.
Not entirely, but the risk can be reduced. For people with high myopia, diabetes, or a family history of retinal detachment, regular eye check-ups are the most important protective measure. If retinal tears or thinning are spotted early during an eye examination, they can often be treated with laser before a detachment develops. Controlling blood sugar in diabetes protects the retina from the changes that lead to tractional detachment. Protecting the eyes from injury is also important.
India has a high and growing burden of two major risk factors: myopia and diabetes. Rising rates of shortsightedness in children and young adults, combined with one of the world’s largest populations of diabetic patients, means that the risk of retinal detachment is a significant public health concern in India. Many cases go undiagnosed until vision is severely affected, because people are not always aware of the warning symptoms or do not have access to regular eye examinations. This is why Vasan Eye Care’s network of 150+ centres across the country plays an important role in bringing timely retinal care closer to communities.
Recovery time varies depending on the type of surgery. After a vitrectomy with a gas bubble, the bubble is gradually absorbed over several weeks, during which the patient may have significantly reduced vision in that eye and must maintain a specific head position. After a scleral buckle, there may be some soreness and swelling for a week or two. In most cases, the operated eye needs several weeks to months before vision stabilises. The doctor will advise on specific restrictions, such as avoiding air travel with a gas bubble inside the eye, which is important because changes in air pressure at altitude can expand the gas and damage the eye.
Other Diseases
Know more about other Eye Diseases
Diabetic Retinopathy
Diabetic Retinopathy happens when high blood sugar levels damage the retinal blood vessels. In the early stages of Diabetic Retinopathy, symptoms may not be noticeable.
Retinopathy Prematurity
Retinopathy Prematurity (ROP) is an eye condition occurring in premature infants, where abnormal blood vessels grow in the retina, potentially resulting in blindness.